Dissecting the immunosuppressive tumor microenvironments in Glioblastoma-on-a-Chip for optimized PD-1 immunotherapy
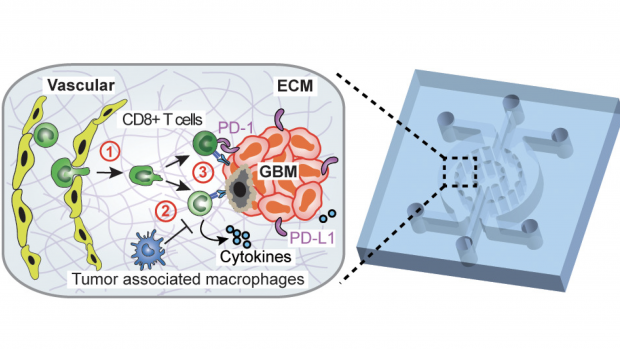
Schematic diagram illustrating a microfluidics-based GBM-on-a-Chip model to investigate the interactions of immune cells (CD8+ T-cells) with brain microvessels, tumor-associated macrophages (TAMs), and GBM tumor cells in an engineered 3D brain-mimicking ECM.
Weiqiang Chen, associate professor of biomedical and mechanical and aerospace engineering led this research.
Glioblastoma (GBM) is the most common and aggressive primary brain tumor among adults, with an average survival of less than 14 months despite aggressive surgery, chemotherapy, and radiotherapy. One of the most promising therapies has been the inhibition of programmed cell death protein-1 (PD-1), which can turn the immune system against the tumors in order to destroy it. However, that approach has been difficult due to the genetic difference between blastomas and the environments they form in.
Improving the clinical use of anti-PD-1 immunotherapy in GBM patients requires a comprehensive understanding of tumor genetics and microenvironment as well as the ability to dissect the dynamic interactions among GBM and immune suppressor cells. Now, a team of researchers led by NTU Tandon’s Weiqiang Chen have integrated critical markers of these microenvironments in a microfluidics-based ex vivo microphysiological system termed ‘GBM-on-a-Chip.’
Modeling the human immune environment in the current animal-based cancer models is challenging. Compared to chemotherapy, it is difficult to preclinically validate and study immunotherapy. Discrepancies between preclinical and clinical results have raised concerns about how the findings from the current models can be translated to patients. The engineered tumor model on chips can be an alternative to the current animal models and patient studies, and even achieve a so-called "clinical trial on chips" for a pre-screening of patients suitable for immunotherapy, and screening personalized therapy for each patient. These chips are patient-specific, allowing longitudinal analysis of cells to understand how the environment around a tumor changes the way that PD-1 cells act.
The team – including researchers from NYU Tandon, NYU Langone Health and NYU School of Medicine, with funding from the National Science Foundation and National Institutes of Health – were able to use the results of this longitudinal study to show that molecularly distinct GBM subtypes have distinct epigenetic and immune signatures that may lead to different immunosuppressive mechanisms. They could see which cells were elevated past their healthy amounts, and which were not responding as they should. This allowed them to administer a specialized treatment for the specific environment, supressing some cells like tumor-associated macrophages while boosting the effectiveness of specific T-cells. Thus, they showed that these patient-specific chips could lead to personalized immunotherapy screening, potentially improving therapeutic outcomes in GBM patients.
The research was conducted with investigators from NYU Tandon, NYU Langone Health, and the NYU School of Medicine.


