Sparse system identification of leptin dynamics in women with obesity
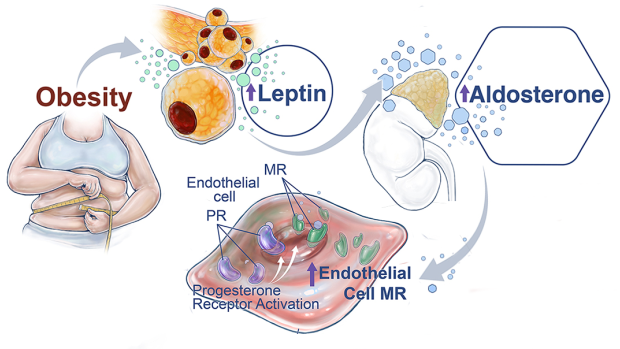
Researchers studying the relationship between leptin and obesity found statistically significant relationships between leptin secretion characteristics and both body mass index (BMI) and lean body mass (LBM).
This research included Rose T. Faghih, Associate Professor of Biomedical Engineering at NYU Tandon, and researchers from the University of Houston, the Louis Bolk Instituut, and the Weill Institute for Neurosciences.
According to the CDC, obesity prevalence in the United States was 42.4 percent in 2017–2018. Obesity prevalence in the United States climbed from 30.5 percent to 42.4 percent between 1999 and 2018. Obesity has been linked to cardiovascular disease, stroke, Type 2 diabetes, and a variety of malignancies. These are some of the most common causes of death that can be avoided. In 2008, the yearly medical cost of obesity in the United States was estimated to reach $147 billion.
It is important to understand the root cause of obesity in terms of hormonal imbalance. To regulate food intake, the brain responds to signals from fat (adipose) tissue, the pancreas, and the digestive tract. These instructions are transmitted via hormones like leptin, insulin, and ghrelin, as well as other small molecules. Among them, leptin is a signaling hormone that is essential to signal the brain in the suppression of appetite. It regulates food intake, metabolism, energy expenditure, and body weight. Thus, leptin regulation is known to be closely related to diseased conditions such as obesity.
In a new study from researchers at NYU Tandon and other schools, the group analyzed the behavior of two neuroendocrine hormones, leptin and cortisol (a stress hormone), in a cohort of patients with obesity. They used a system theoretic approach that can accurately estimate the internal secretion patterns, timings, amplitudes, number of underlying hormone secretory pulses, infusion, and clearance rates of hormones in patients with obesity by only measuring the 24-hour blood assay of their hormones.
The findings suggest a method for mathematically modeling both leptin and cortisol hormones to characterize how they interact as part of a larger system. Because the relationship between leptin and cortisol hormones is complex, the new results and projections will help us understand how these hormones work together to keep the body in a state of homeostasis.
The researchers demonstrated a negative relation between leptin and cortisol secretion, based on a statistical test called the Granger causality test among the patients with obesity. These results indicate that increases in cortisol are prospectively associated with reductions in leptin, suggesting a negative inhibitory relationship in 14 out 18 obese women investigated. Reduced leptin may result in a decrease in satiety and thereby lead to obesity
The model can be a crucial contribution toward the potential development of the next generation of agile closed-loop medical systems related to obesity. Such next-generation closed-loop medical systems will identify deviations from homeostasis and suggest necessary interventions benefiting from regular tracking of hormone secretory events and underlying endocrinological system parameters. This way complex conditions such as obesity can be prevented at the root level resulting in an overall increase in the quality of life and reduction in the total national medical expenditure.




