Mending Broken Hearts
Assistant Professor Irene de Lázaro is on the path to regenerating damaged cardiomyocytes in vivo
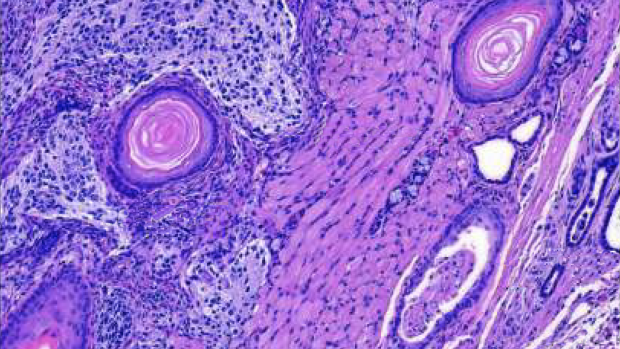
H&E stained section of a heart showing evidence of cardiomyocyte reprogramming
If you cut yourself, you will probably heal readily, since skin cells have the ability to regenerate. That’s not true, however, of the more than two billion cardiac muscle cells in the human heart, since most of those cells, known as cardiomyocytes, lose the ability to divide soon after we are born. That means that someone who suffers a heart attack, for example, will not grow new cells to replace those that die.

NYU Tandon Assistant Professor of Biomedical Engineering Irene de Lázaro is working to change that situation. She first became interested in the topic of tissue regeneration while earning a master’s degree in Drug Delivery at University College London’s School of Pharmacy and reading about “cellular reprogramming,” a technique by which forced expression of a group of genes that are highly expressed in the embryonic stages of development, but not later, can make an adult cell behave like an embryonic stem cell. This includes its ability to divide and also to re-differentiate again into virtually any cell type of the body. (Gene expression refers to the process in which the information encoded in a gene is used to direct the assembly of a functional product, such as a protein.)
De Lázaro — who, in addition to her post at Tandon, is now a member of NYU's Cardiovascular Research Center and holds a cross-appointment to Langone’s Division of Cardiology — subsequently remained at University College London to study for a Ph.D. in Regenerative Medicine and work with a research group dedicated to pioneering in vivo cellular reprogramming — a clear leap forward, since until then this technique had only been demonstrated in vitro.
It’s now possible, she has explained, to reprogram a cell either all the way back to the embryonic stage or to a somewhat earlier stage in which they’re rejuvenated and behave as a younger cell would. But while it may sound to the layperson as though scientists had discovered a veritable fountain of youth or developed the ability to build fully functioning human organs in the lab, de Lázaro cautions that the work is still in its basic, foundational stages and that human trials are likely to be several years away, only after key safety concerns are addressed. “It’s too soon to predict an exact timeline,” she says, “but I feel very hopeful we’re moving in the right direction.”
The students in her graduate Tissue Engineering course, she asserts, just may be in the next generation of biomedical engineers, capable of regenerating or building entire working organs in their labs one day, healing hearts and other vital body parts thanks to cell-reprogramming technology.
To learn more about post-doctoral opportunities in the de Lázaro Lab, contact irene.delazaro@nyu.edu.




